As a blogger, I'm excited to share some insights on the future of vascular disease treatment, which is a rapidly evolving field. Emerging therapies and ongoing research are paving the way for more effective and less invasive treatments. Breakthroughs such as drug-coated balloons, bioresorbable stents, and gene therapy show great potential in addressing various vascular conditions. Additionally, advancements in imaging technology are set to significantly improve the accuracy and efficiency of diagnosis. Overall, these innovations will revolutionize the way we treat vascular diseases and improve the quality of life for millions of patients.
Vascular disease treatment: practical options and what to ask your doctor
Vascular disease covers problems with arteries and veins—like peripheral artery disease, carotid artery narrowing, aneurysms, and chronic venous insufficiency. Treatment aims to reduce symptoms, prevent stroke or amputation, and lower heart attack risk. Here are clear, practical options so you know what to expect and what to discuss with your clinician.
First-line steps are lifestyle changes.
Quit smoking, control blood pressure, lose weight when needed, and get regular exercise. A supervised walking program helps peripheral artery disease more than casual activity. Eating a Mediterranean-style diet lowers cholesterol and inflammation. These steps are not optional; they change outcomes.
Medications play a big role.
Antiplatelet drugs such as aspirin or clopidogrel cut stroke and clot risk. Statins lower LDL cholesterol and stabilize plaques. Blood pressure medicines—ACE inhibitors, ARBs, or calcium channel blockers—protect arteries and the heart. For deep vein thrombosis or certain high-risk artery clots, short- or long-term anticoagulants like warfarin or direct oral anticoagulants are used. Always ask about bleeding risks and drug interactions, especially with herbal supplements.
Endovascular and surgical treatments are options when meds and lifestyle aren’t enough. Angioplasty with stent placement opens narrowed arteries in the leg or neck. Carotid endarterectomy removes dangerous plaque in carotid arteries to prevent stroke. Bypass surgery reroutes blood around blocked vessels. For aneurysms, endovascular repair or open surgery prevents rupture. Ask your surgeon about success rates, recovery time, and what complications to watch for.
Vein problems need different care. Compression stockings, leg elevation, and weight loss ease chronic venous insufficiency. For varicose veins, minimally invasive procedures—laser, radiofrequency ablation, or foam sclerotherapy—work well and recover fast. For a blood clot in a deep vein, early anticoagulation is the usual step.
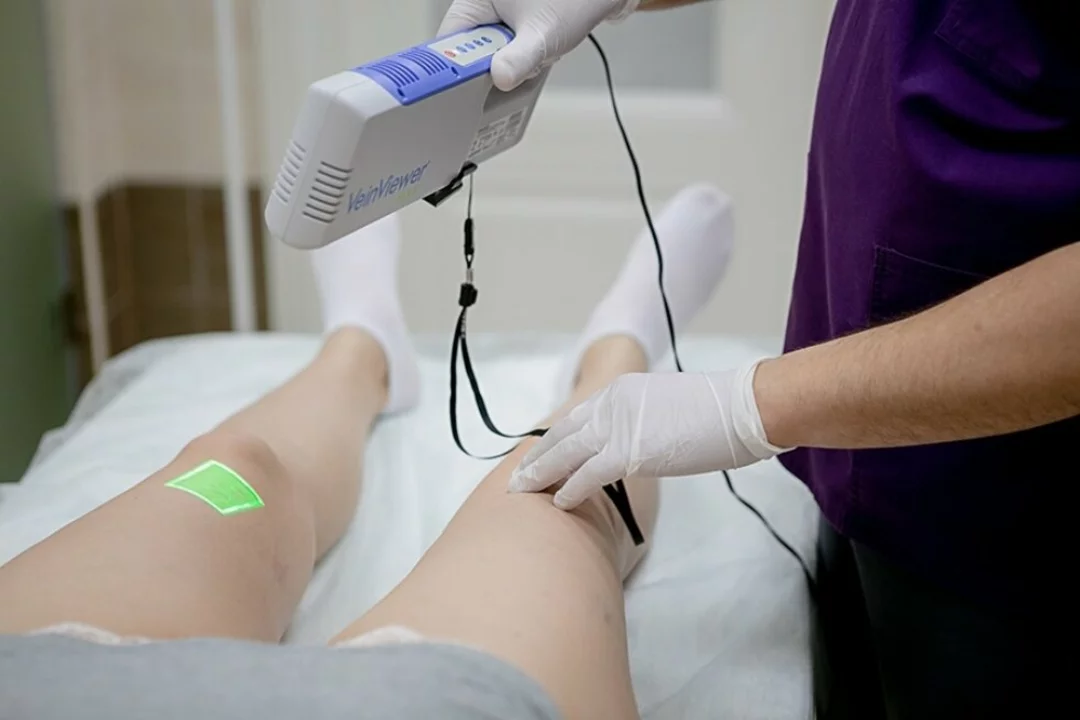
Monitoring and follow-up matter. Regular imaging—ultrasound, CT angiography, or MR angiography—tracks disease progress and treatment success. Routine blood tests check cholesterol levels and medication safety. Keep a log of symptoms, walking distance, and any new numbness or weakness to share with your team.
Questions to ask your doctor: What is my specific vascular diagnosis and severity? Could I try lifestyle changes first? Which medicines do you recommend and why? Am I a candidate for a procedure or surgery? What are the risks and recovery expectations? How often will I need follow-up tests?
If you have diabetes or kidney disease, treat those conditions aggressively; they raise vascular risk. Don’t delay care for new limb pain, sudden weakness, speech trouble, or signs of a clot. Faster treatment often prevents permanent damage.
Practical tips: take medicines at the same time each day and use a pillbox or app to avoid missed doses. Join a smoking-cessation program. If you have leg pain when walking, measure how far you go and bring that number to appointments. Wear shoes and inspect feet if you have diabetes. Seek urgent care for sudden chest pain or stroke signs.
This tag page gathers practical articles on medications, procedures, and recovery tips to help you make smarter choices about vascular disease treatment.