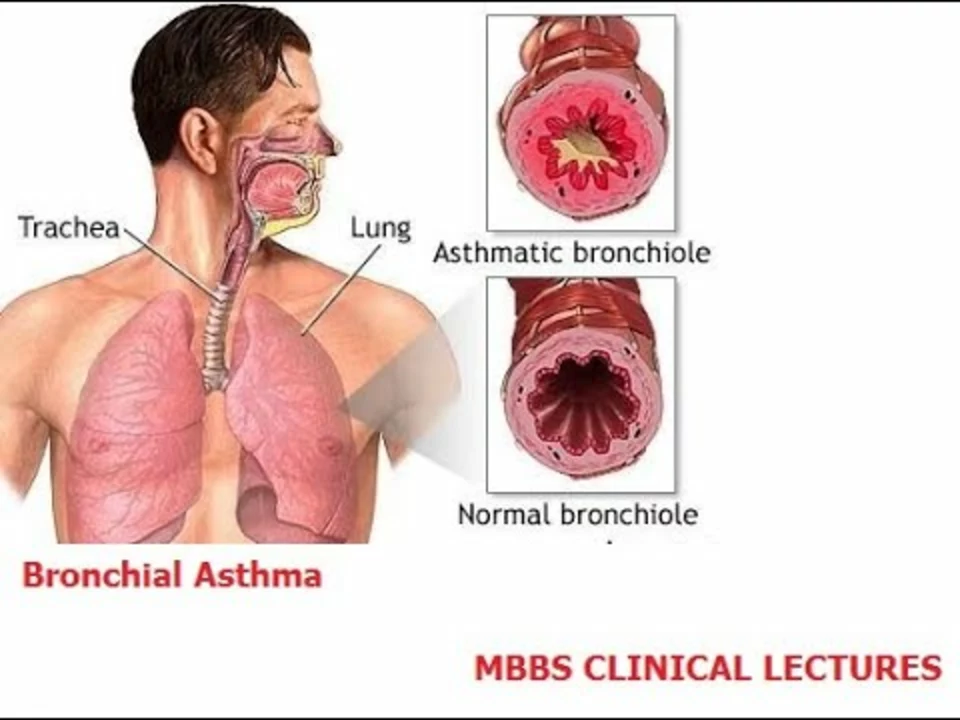
As a blogger, I've been exploring the role of environmental factors in bronchial asthma. I've discovered that exposure to allergens, air pollution, and tobacco smoke can significantly contribute to this condition. Moreover, climate change as well as indoor environments like mold and dust mites also play a part in triggering asthma symptoms. It's important to be aware of these factors in order to better manage and prevent asthma attacks. By understanding the environmental impact on bronchial asthma, we can take steps to create healthier living spaces for those suffering from this condition.
Bronchial Asthma: Practical Tips to Breathe Easier
Bronchial asthma causes wheeze, cough, chest tightness and shortness of breath. If you have asthma, you already know symptoms come and go. This page gives clear, practical steps you can use today to reduce attacks, handle flare ups and talk to your doctor smarter.
Start by spotting triggers. Common ones are pollen, dust mites, pets, cold air, smoke, strong smells, exercise and viral infections. Keep a simple diary for two weeks: note symptoms, where you were and what you did. That short habit often shows one or two avoidable triggers fast.
Inhalers are the main tool. Short acting beta agonists like salbutamol (Ventolin) stop acute breathlessness in minutes. Inhaled corticosteroids reduce inflammation and lower future risk when used regularly. If you're unsure how to use an inhaler, ask for a demonstration and try a spacer—it improves delivery and cuts side effects.
Daily control and monitoring
Make a routine. Take controller medicine every day if prescribed, even on good days. Use a peak flow meter at home to watch trends; a drop of 20 percent from your personal best often signals a worsening problem. Create a written action plan with three zones—green (stable), yellow (worse), red (emergency)—so you know exactly what medicine to take and when to call for help.
Know when to seek help. If you can’t speak full sentences, your lips or face look blue, your peak flow is in the red zone or symptoms don’t improve after using your reliever inhaler, get emergency care now. Faster response reduces the chance of hospitalization.
Treatment options and questions to ask
Besides relievers and inhaled steroids, options include long acting bronchodilators, leukotriene modifiers and biologic injections for severe allergic types. For mild cases, some people explore herbal bronchodilators or supplements—talk with your clinician first because herbs can interact with medicines. Ask these questions at your next visit: what’s my trigger plan, how and when should I step up treatment during a flare, and can I reduce steroid dose once controlled?
Practical everyday tips: wash bedding in hot water weekly to cut dust mites, avoid smoking and smoky places, warm up before exercise if exercise triggers you, and keep vaccines up to date—especially flu and COVID shots. Plan travel with extra inhalers and copies of prescriptions; store medicines in carry‑on luggage.
Finally, people with asthma do well when they learn the pattern of their disease. Track symptoms, keep meds handy, and check in regularly with your provider. If attacks are frequent despite treatment, ask about specialist referral—the right plan can change your life.
Want more practical reading? Check our piece on herbal bronchodilators for what works and what doesn’t, plus a travel guide for people with obstructive lung disease. Use those articles to prepare for conversations with your doctor. Small changes —like better inhaler technique, trigger control and timely vaccination— add up fast and help you breathe easier every day.
Remember, asthma management is personal; keep learning, adapting, and asking questions until you feel confident.