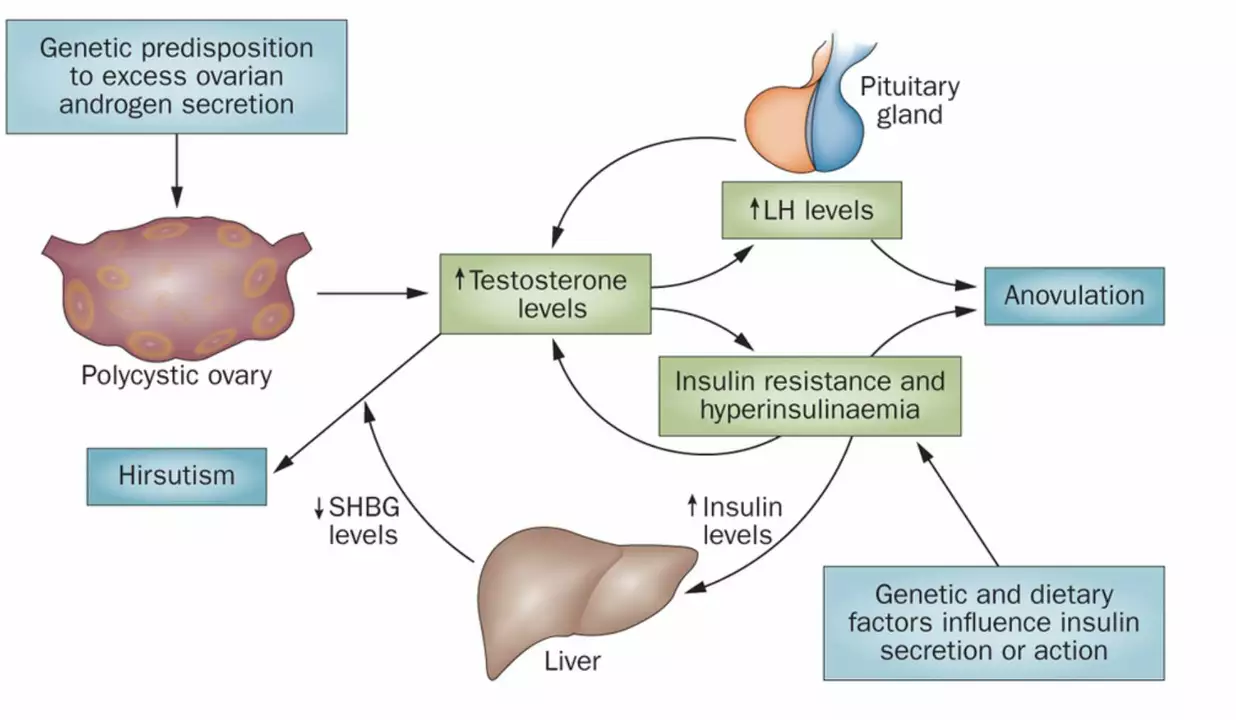
As someone who has been researching Polycystic Ovary Syndrome (PCOS), I've discovered a strong connection between this condition and infertility. PCOS is a hormonal disorder that affects up to 10% of women of reproductive age, causing irregular menstrual cycles and elevated levels of male hormones. Due to these imbalances, ovulation becomes irregular or absent, making it difficult for women with PCOS to conceive naturally. Additionally, the syndrome can lead to insulin resistance, weight gain, and other health issues that further complicate fertility. Overall, understanding and managing PCOS is crucial for women who are struggling with infertility, as it can significantly impact their chances of becoming pregnant.
PCOS: What to watch for and what actually helps
PCOS (polycystic ovary syndrome) shows up as missed periods, heavy or irregular cycles, excess hair, acne, or trouble getting pregnant. It also often means higher insulin and sometimes weight gain. If that sounds familiar, you don’t need confusion — just a clear plan: confirm the diagnosis, treat the symptoms that bother you, and focus on changes that improve long-term health and fertility.
How doctors diagnose PCOS
Most clinicians use the Rotterdam rules — you need two of three: irregular ovulation, high male hormones on blood tests or visible signs like acne/hirsutism, and polycystic-looking ovaries on ultrasound. Useful tests: fasting glucose and insulin, HbA1c, lipid profile, testosterone, LH/FSH, and pelvic ultrasound. AMH (anti-Mullerian hormone) can help estimate ovarian reserve and support the diagnosis but isn’t required for everyone.
If labs show insulin resistance, that alters the plan. High insulin often drives symptoms and raises long-term risks like type 2 diabetes. Get baseline bloodwork so treatment can be targeted and safe.
Practical steps that help right away
Small, consistent changes move the needle. Losing 5–10% of body weight often restores periods and improves ovulation for folks with overweight. Focus on a lower-refined-carb, whole-food pattern (Mediterranean-style works well), regular strength training and walking, and consistent sleep. These things improve insulin sensitivity and lower testosterone symptoms.
Medication choices depend on goals. For cycle control and acne, combined birth control pills and anti-androgens work for many. If you want to get pregnant, letrozole is now the first-line ovulation drug for many people with PCOS — studies show better live-birth rates than clomiphene (Clomid). Other fertility options include gonadotropin injections, timed intercourse with monitoring, intrauterine insemination (IUI), and IVF if needed. Surgical ovarian drilling is rarely used but can help some people who don’t respond to meds.
Metformin can help when insulin resistance is present — it can improve cycles and reduce diabetes risk. Supplements with some supporting evidence include myo-inositol (for ovulation and insulin) and vitamin D if deficient. Some people ask about calcium D-glucarate or chitosan; these have limited evidence for hormone balance or weight loss and should be discussed with your clinician before use.
Monitor treatment: if you’re on ovulation induction, expect ultrasound monitoring and hormone checks to avoid multiple pregnancy risks. If using prescription meds, track side effects and routine labs as your doctor recommends. If fertility treatment isn’t moving forward after several cycles, ask for a fertility referral — timelines differ by age and individual factors.
PCOS is manageable with the right tests, targeted treatment, and lifestyle steps you can stick with. Start by getting clear lab results and a treatment goal (cycle regularity, acne control, or pregnancy) — that makes the next steps obvious and practical.