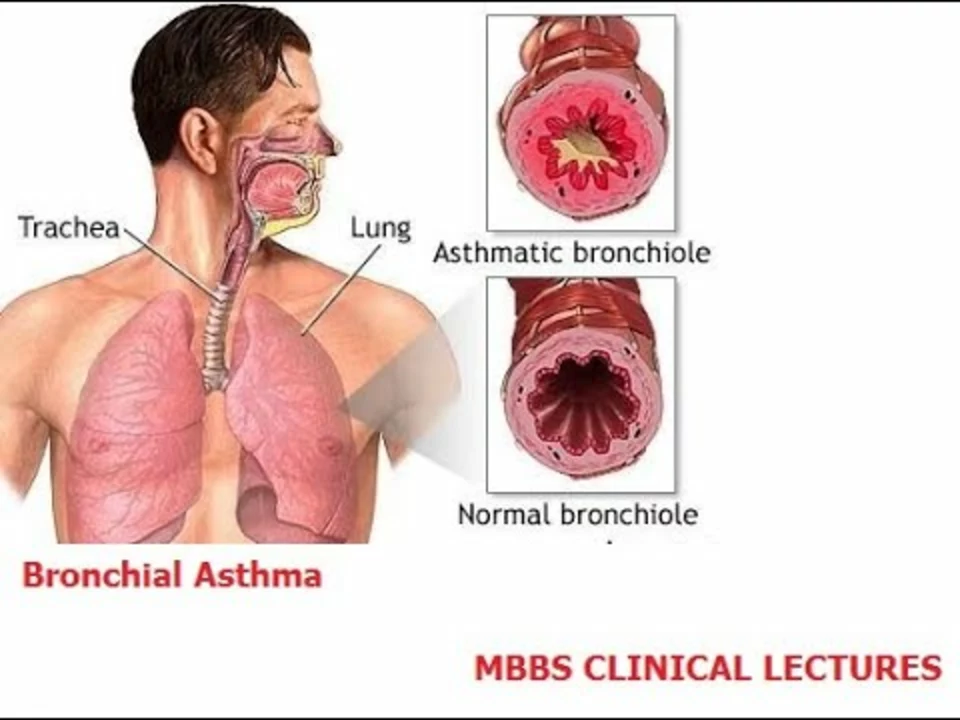
As a blogger, I've been exploring the role of environmental factors in bronchial asthma. I've discovered that exposure to allergens, air pollution, and tobacco smoke can significantly contribute to this condition. Moreover, climate change as well as indoor environments like mold and dust mites also play a part in triggering asthma symptoms. It's important to be aware of these factors in order to better manage and prevent asthma attacks. By understanding the environmental impact on bronchial asthma, we can take steps to create healthier living spaces for those suffering from this condition.
Environmental factors: how air, climate & your surroundings affect health
Want to know why your asthma flares up on some days and not others? Or why a medicine you tolerate at home makes you feel worse while traveling? The environment around you — air quality, humidity, temperature, chemicals and even noise — can change how you feel and how medicines work. This page explains the main risks and gives simple, useful things you can do right away.
Everyday environmental risks that change your health
Air pollution and tiny particles (PM2.5) can irritate lungs, trigger asthma or make COPD worse within hours. If you notice more coughing on smokey or dusty days, that’s the likely cause. Indoor allergens — dust mites, mold, pet dander — can make allergies and eczema flare. Damp homes and poor ventilation help mold grow fast.
Heat and cold matter too. Heat waves raise the risk of dehydration, fainting, and problems for people on diuretics or some heart medicines. Cold can stiffen blood vessels and make breathing harder for some lung conditions. Some drugs increase sun sensitivity (for example, certain antibiotics and acne meds) so you burn more easily on sunny days.
Work and hobby exposures count: solvents, strong cleaning chemicals, and pesticides can cause skin or breathing problems. Noise and light pollution affect sleep, and chronic poor sleep worsens mental health, pain, blood pressure and recovery from illness.
Simple, practical steps to protect yourself
Check the air quality index (AQI) in your area before going out. On high-pollution days, avoid heavy exercise outdoors or move activities inside. Use an N95 mask in smoky or dusty conditions if you must be outside for long periods.
Reduce indoor triggers: run a HEPA air cleaner in bedrooms, keep indoor humidity around 40–50% to slow mold and dust mites, wash bedding weekly in hot water, and fix leaks quickly. Avoid strong chemical sprays; choose unscented, low-VOC cleaning products when possible.
Protect your skin and meds: wear sunscreen and protective clothing if your medicine can cause photosensitivity. Keep medicines stored at recommended temperatures — extreme heat or cold can change how well they work. When traveling to high altitudes or very hot places, ask your pharmacist if your meds need dose changes or extra monitoring.
If you work with chemicals, use gloves, goggles, and proper ventilation. For noisy jobs, use ear protection. Small habits add up — staying hydrated, getting consistent sleep, and washing hands reduce many environment-linked risks.
Notice a pattern? Track symptoms against weather, AQI, or activities for a week or two. Bring that info to your doctor or pharmacist — it makes advice more useful and quicker. If an exposure causes sudden breathing trouble, chest pain, severe rash, or confusion, get medical help right away.
Want more specific tips for a condition (asthma, skin issues, or medication safety)? Search our site or reach out to a pharmacist for tailored advice.