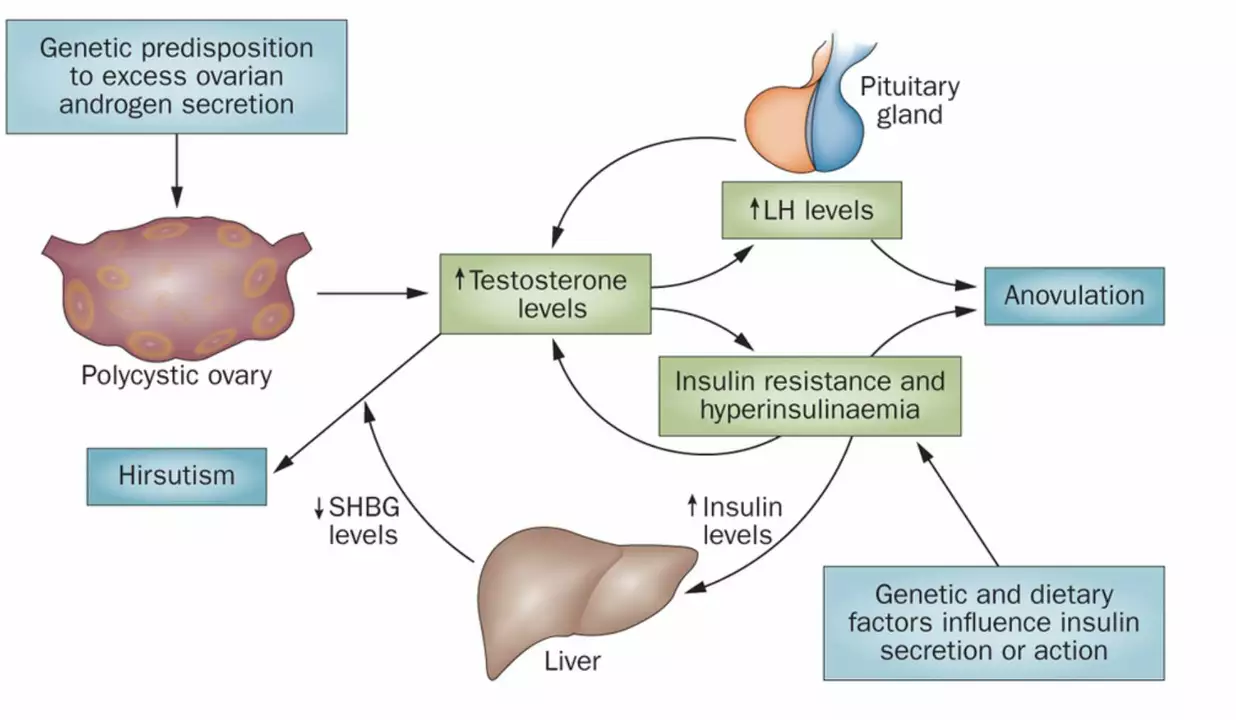
As someone who has been researching Polycystic Ovary Syndrome (PCOS), I've discovered a strong connection between this condition and infertility. PCOS is a hormonal disorder that affects up to 10% of women of reproductive age, causing irregular menstrual cycles and elevated levels of male hormones. Due to these imbalances, ovulation becomes irregular or absent, making it difficult for women with PCOS to conceive naturally. Additionally, the syndrome can lead to insulin resistance, weight gain, and other health issues that further complicate fertility. Overall, understanding and managing PCOS is crucial for women who are struggling with infertility, as it can significantly impact their chances of becoming pregnant.
Infertility: Practical Answers and Real Next Steps
About 1 in 6 couples has trouble getting pregnant. That stat feels huge when it’s you, but knowing clear next steps makes a big difference. Below you’ll find simple, practical advice—what tests to expect, what treatments actually do, and how to choose medications like Clomid or its alternatives.
When to see a specialist and what they’ll check
If you’re under 35 and haven’t conceived after a year of trying, or over 35 and haven’t conceived after six months, see a fertility specialist. The first visit is short on drama and long on tests: ovulation tracking, hormone blood tests (FSH, AMH, TSH), a hysterosalpingogram to check tubes, and a semen analysis for your partner. These tests tell whether the issue is ovulation, blocked tubes, sperm quality, or a mix.
Getting tests early saves time and money. If tests show a clear cause, treatment often follows a straightforward path. If they’re normal, your doctor will explain options like timed intercourse, intrauterine insemination (IUI), or IVF.
Common treatments, meds, and what to expect
First-line for ovulation problems often starts with oral meds. Clomid (clomiphene) has been common for years. In many cases, letrozole—an aromatase inhibitor—works equally well or better, especially for people with PCOS. If oral meds don’t work, doctors may suggest injectable gonadotropins. These are stronger, need monitoring with ultrasounds and bloodwork, and raise the chance of multiple pregnancy, so expect careful follow-up.
IUI can be a next step when sperm quality is a mild issue or ovulation meds are used. IVF is the most effective route for many problems: blocked tubes, severe male factor, or when other steps fail. IVF gives the most control but costs more and requires more time and tests.
Side effects matter. Clomid can cause mood swings and hot flashes; letrozole may cause fatigue or joint pain; injectables can cause ovarian hyperstimulation in some people. Your team will explain risks, monitoring, and how to reduce side effects.
Don’t forget simple, evidence-backed changes that help: stop smoking, cut excess alcohol, aim for a healthy BMI, and take a prenatal vitamin with folic acid. For men, improving sleep, avoiding hot tubs, and limiting heavy alcohol can boost sperm quality.
If cost or side effects push you away from one option, there are alternatives. Articles on this site cover practical lists of Clomid alternatives, how gonadotropins differ, and when to consider referral for IVF. Use those guides when you compare costs, success rates, and side effects.
Finally, keep communication open with your partner and care team. Infertility care moves in steps—test, try the least invasive option that fits your situation, then escalate if needed. Small, clear steps usually lead to the best outcomes and keep stress lower along the way.