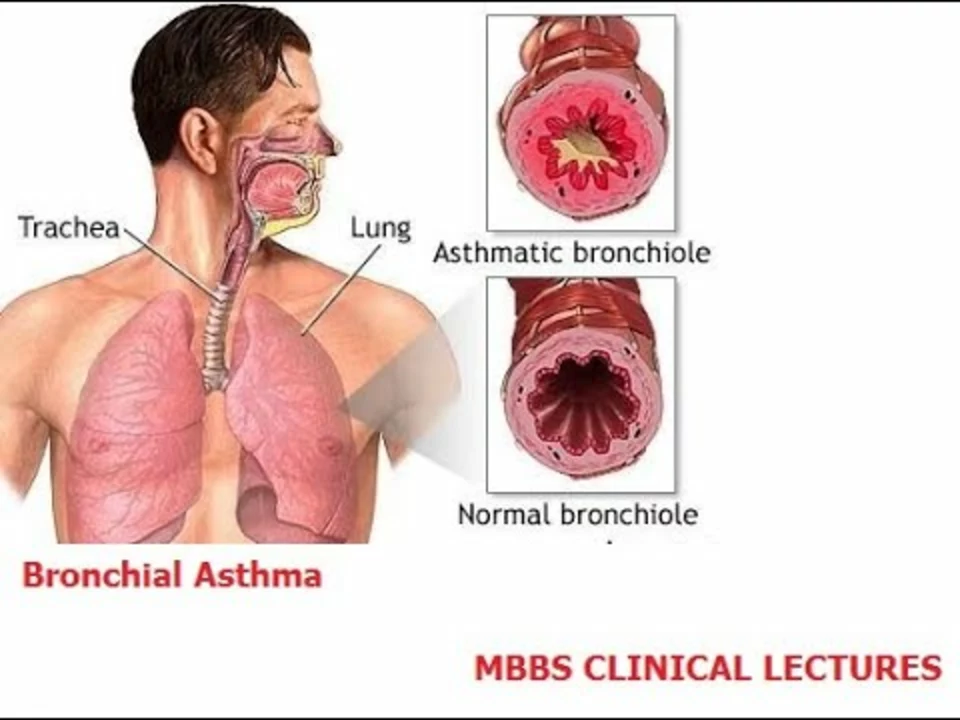
As a blogger, I've been exploring the role of environmental factors in bronchial asthma. I've discovered that exposure to allergens, air pollution, and tobacco smoke can significantly contribute to this condition. Moreover, climate change as well as indoor environments like mold and dust mites also play a part in triggering asthma symptoms. It's important to be aware of these factors in order to better manage and prevent asthma attacks. By understanding the environmental impact on bronchial asthma, we can take steps to create healthier living spaces for those suffering from this condition.
Asthma Triggers: How to Spot and Stop What’s Making You Wheeze
If your chest tightens at night, after cleaning, or during a run, a trigger is usually behind it. Knowing the most common triggers and simple ways to reduce exposure can cut attacks and help you breathe easier every day.
Common asthma triggers
Here are the triggers I see most often, and what they actually do to your lungs:
- Allergens: Dust mites (in pillows and mattresses), pet dander, cockroaches, and pollen. These cause inflammation and wheeze days after exposure.
- Smoke and fumes: Tobacco smoke, wood smoke, and strong chemical smells (paints, cleaning sprays, perfume) can irritate airways instantly.
- Exercise and cold air: Hard exercise, especially in cold or dry weather, can trigger bronchospasm within minutes.
- Respiratory infections: Colds and flu are major triggers—your airways get inflamed and more reactive.
- Medications and health conditions: Some people react to aspirin or NSAIDs. Acid reflux (GERD) can also worsen asthma symptoms, especially at night.
- Stress and strong emotions: Intense laughter, crying, or anxiety can lead to rapid breathing and trigger symptoms.
How to reduce exposure & practical tips
Start with small, doable changes that cut daily exposure:
- Use allergen-proof mattress and pillow covers and wash bedding in hot water weekly to kill dust mites.
- Keep pets out of the bedroom and groom them outside. If symptoms persist, consider limiting indoor pet access.
- Quit smoking and avoid secondhand smoke. Don’t allow vaping or smoking in your home or car.
- Use unscented cleaning products. Open windows or use a mask when painting or using strong cleaners.
- Before exercise, use your quick-relief inhaler 10–15 minutes ahead if your doctor recommends it. Warm up slowly and cover your mouth in cold weather.
- Get flu and COVID vaccines and teach kids good hand hygiene to reduce infection risk.
- Run a HEPA air filter in the bedroom if pollen or smoke is a problem. Keep indoor humidity around 30–50% to limit mold.
- If GERD is an issue, avoid late large meals, reduce caffeine and spicy foods, and raise your bed head slightly.
Keep an asthma action plan from your doctor. Know your personal warning signs: needing your rescue inhaler more often, waking at night with symptoms, or lower peak flow readings. These mean you should change treatment or see your clinician.
Emergency signs include severe breathlessness, blue lips, trouble speaking, or poor response to your reliever inhaler—call emergency services immediately. With the right trigger control and a clear action plan, most people can reduce attacks and stay active without fear.