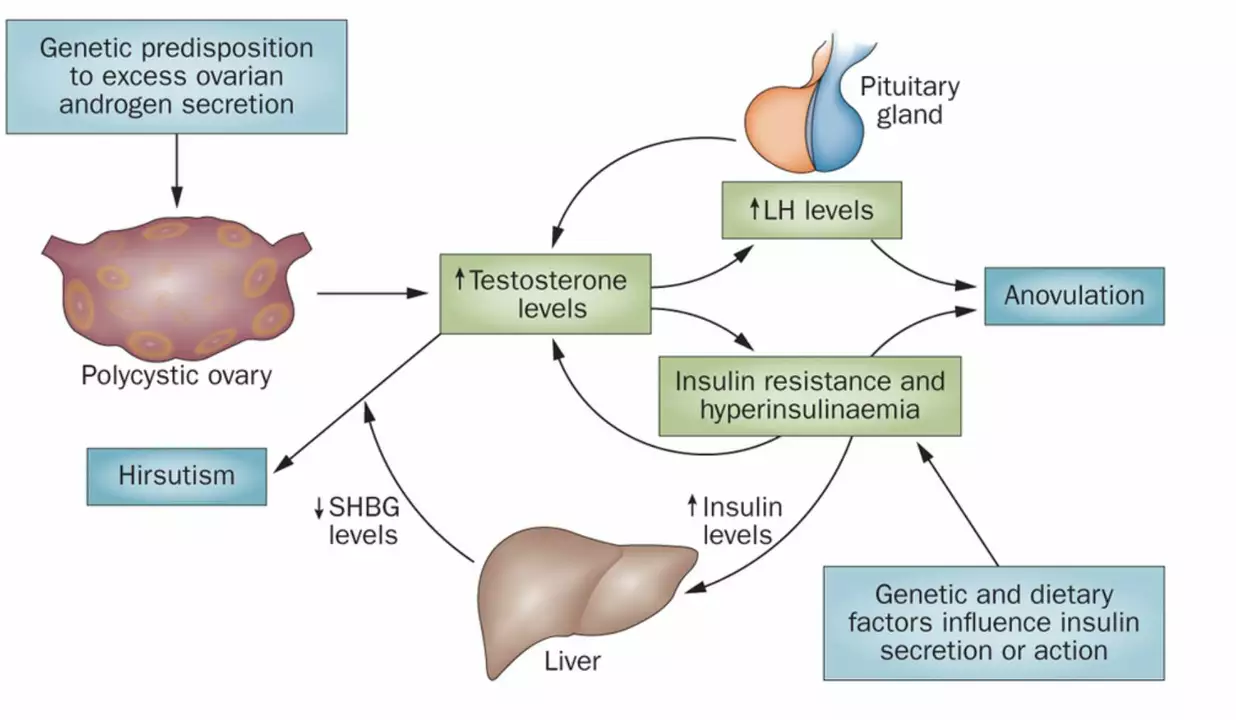
As someone who has been researching Polycystic Ovary Syndrome (PCOS), I've discovered a strong connection between this condition and infertility. PCOS is a hormonal disorder that affects up to 10% of women of reproductive age, causing irregular menstrual cycles and elevated levels of male hormones. Due to these imbalances, ovulation becomes irregular or absent, making it difficult for women with PCOS to conceive naturally. Additionally, the syndrome can lead to insulin resistance, weight gain, and other health issues that further complicate fertility. Overall, understanding and managing PCOS is crucial for women who are struggling with infertility, as it can significantly impact their chances of becoming pregnant.
Ovary syndrome: signs, tests, and practical steps
Worried about irregular periods, sudden weight gain, or extra facial hair? Those are common clues people call "ovary syndrome," often meaning polycystic ovary syndrome (PCOS). It’s not one single problem — it’s a pattern of symptoms tied to hormones. You don’t need to panic, but getting the right checks and small changes early can make a big difference.
Spotting the symptoms
Look out for a few clear signs: irregular or missed periods, heavy bleeding, trouble getting pregnant, acne that won’t clear, unwanted hair growth on the face or body, and unexplained weight gain or difficulty losing weight. Some people also feel fatigued or notice mood swings. If you have two or more of these issues, it’s reasonable to talk to a clinician about PCOS or other ovarian problems.
Another common symptom is ovarian pain or discomfort during your cycle. If pain is sharp, worsening, or accompanied by fever or fainting, seek urgent medical care — that could mean something more than a hormonal condition.
What doctors check and simple next steps
A typical evaluation starts with a clear history and a pelvic exam. Blood tests often measure hormones (like LH, FSH, testosterone), thyroid function, and blood sugar or insulin markers. An ultrasound looks for ovarian cysts or other structural issues. No single test proves PCOS — doctors use the overall picture.
Treatment depends on your goals. Want to regulate periods or reduce acne? Birth control pills or anti-androgen medications are commonly used. Trying to conceive? Medications like letrozole are often recommended; clomid and other options exist, too. For insulin resistance or weight management, doctors may suggest lifestyle changes and sometimes metformin. Always discuss risks and benefits with your provider before starting any medication.
Simple steps you can start now: track your menstrual cycles, keep a food-and-exercise log for a few weeks, and write down your main concerns (fertility, acne, weight, or hair). Bring that list to your appointment — it makes the visit far more productive.
Lifestyle changes do help many people: modest weight loss (5–10% if overweight), balanced meals with fewer refined carbs, and regular activity can improve symptoms and insulin sensitivity. These are practical, low-risk steps you can begin before or alongside medical treatments.
Want quick reads from our site? Check these helpful articles: “2025's Top Alternatives to Clomid” for fertility options, “Letrozole vs Tamoxifen” to understand letrozole’s role, and “Calcium D-Glucarate” for a look at a supplement people use for hormone balance. Each gives practical, easy-to-follow info you can discuss with your doctor.
If you suspect ovary syndrome, book a visit with a gynecologist or endocrinologist. Clear testing and a straightforward plan will put you back in control — and most people see real improvements once they start the right steps.